Botox® in Clinical Practice: Patient Selection, Technique, and Safety
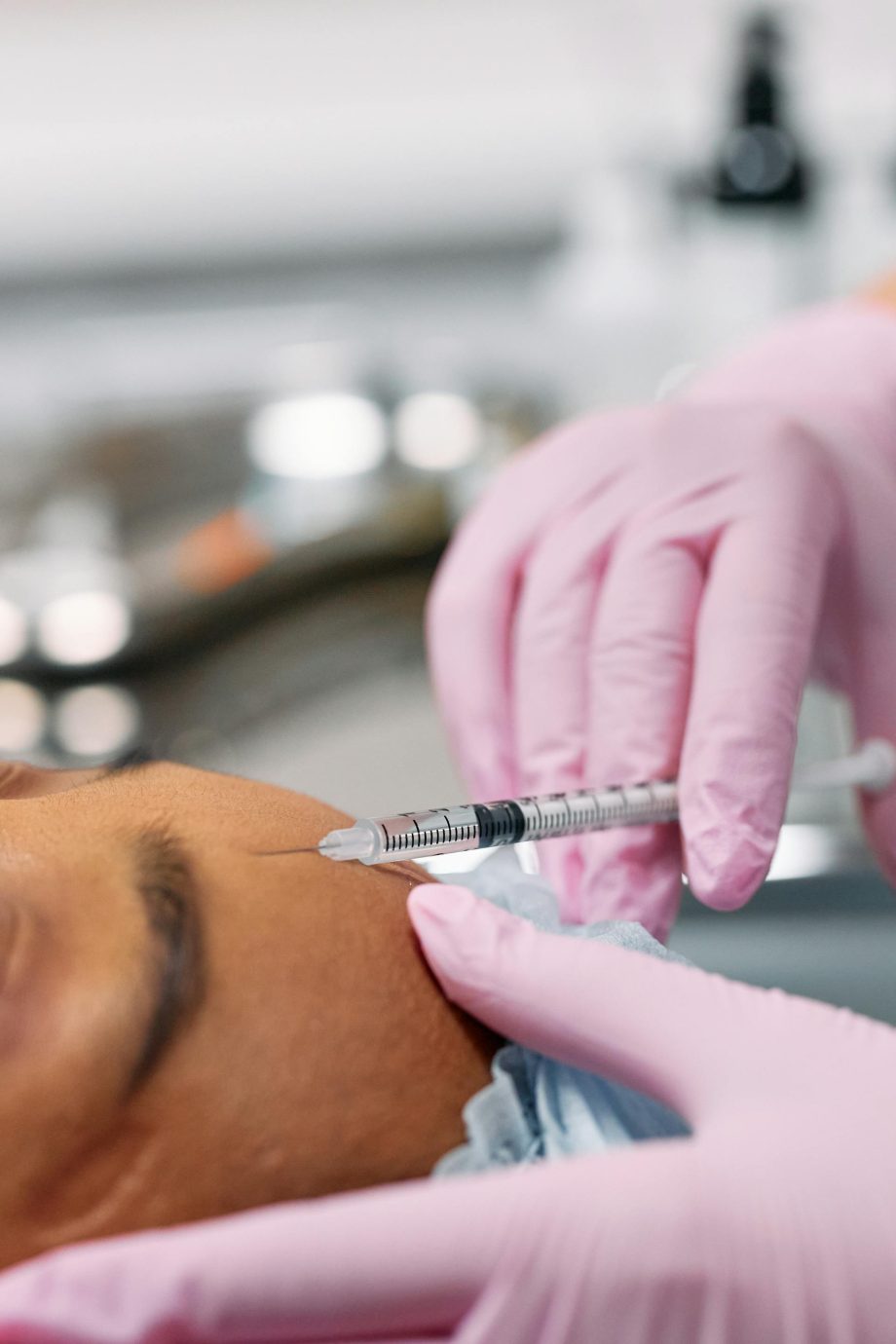
Facial lines, chronic migraine, and focal muscle overactivity affect daily function. Many patients seek durable relief with minimal downtime. Botox® is often part of a multimodal plan, provided expectations and safety are aligned.
For a concise page summarizing formulation and clinical context, review the Botox Product Page before discussing patient-specific details. The information below supports clinical decision-making, including assessment, dosing considerations, and follow-up strategies.
Clarifying Indications and Patient Goals
Start by mapping symptoms to functional impact. For aesthetic concerns, identify dynamic versus static lines. Dynamic lines deepen with movement; static lines persist at rest. For movement disorders or spasticity, document distribution, severity, and triggers. In migraine, track headache days, associated symptoms, and disability scores.
Set goals that are measurable and time-bound. Examples include softening glabellar frown intensity, reducing axillary sweat episodes, or improving wrist hygiene in upper-limb spasticity. Align goals with realistic onset and duration windows. Patients often expect rapid, permanent results; explain that effects emerge gradually and wane over months.
Mechanism and Expected Response
Botulinum neurotoxins act at the neuromuscular junction to reduce acetylcholine release. This temporarily decreases muscle contraction or glandular activity. Peak effect typically appears within two weeks, with a gradual taper thereafter.
Response varies by muscle size, baseline activity, and dose distribution. Reinforce that touch-ups should respect appropriate intervals to lower cumulative risk. For chronic conditions, plan cyclical reassessment to gauge benefit and adjust patterns.
Assessment and Planning
History and Examination
Gather medical, neuromuscular, and autonomic histories. Screen for neuromuscular junction disorders, bleeding risk, active infection at planned sites, and pregnancy or lactation status. List current agents that may potentiate weakness, such as aminoglycosides or muscle relaxants.
Examine at rest and with activation. Map hyperfunctional lines, muscle bulk, and asymmetries. For spasticity, document Modified Ashworth Scale scores, range-of-motion limits, and functional tasks. For hyperhidrosis, quantify affected areas and triggers; consider starch-iodine testing when practical.
Injection Design
Plan a grid or anatomic map before reconstitution. Prioritize lower effective doses in smaller or balance-critical muscles, such as periorbital and perioral regions. Avoid diffusion into antagonists essential for function. In limb spasticity, use EMG or ultrasound guidance when muscle boundaries are uncertain.
Individualize dilution to support precise aliquots and coverage. Communicate expected onset and possible staged treatments to meet goals while limiting adverse effects.
Technique and Practical Tips
- Preparation: Use aseptic technique; confirm product integrity and lot-tracking. Reconstitute gently to reduce foaming.
- Anatomy: Palpate and mark in neutral and active states. In the upper face, respect brow depressor“elevator balance to avoid ptosis or brow drop.
- Needle selection: Choose gauge and length appropriate to depth. Superficial placement for lines; deeper intramuscular placement for bulkier targets.
- Dose spacing: Distribute micro-aliquots to reduce diffusion. Reserve cautious higher dosing for larger muscles or refractory patterns.
- Pain control: Ice, vibration, or topical anesthetic can improve tolerance. Consider pre-procedure counseling for needle-averse patients.
- Documentation: Record sites, doses, dilution, guidance modality, and observed anatomy. Use face or limb maps to facilitate reproducibility.
Monitoring Outcomes and Adverse Effects
Track onset, peak, durability, and functional gains. Photographs or standardized scales help objectify change. For migraine, use headache diaries and disability scores to evaluate benefit over cycles.
Common transient effects include injection-site pain, bruising, and localized weakness. Ocular treatments risk ptosis or diplopia from diffusion. Perioral injections can affect articulation or oral competence. Cervical injections may cause neck weakness; counsel accordingly.
Less common but serious risks include systemic spread symptoms like dysphagia or dyspnea. Educate patients on red flags and when to seek urgent care. Avoid treating when infection is present at the target site.
Expectations, Counseling, and Follow-Up
Set the timeline clearly: partial effect in several days, peak around two weeks, and gradual decline thereafter. Emphasize that correction is not permanent and repeat sessions may be needed. Over-correction can be functionally limiting, especially around the eyes and mouth.
Schedule follow-up at two to four weeks for first-time patients. Early review supports minor adjustments while respecting cumulative dosing constraints. For established regimens, evaluate at each cycle and recalibrate mapping as anatomy or goals change.
Integrating with Multimodal Care
For spasticity, combine injections with stretching, splinting, and task-specific therapy. Collaboration with rehabilitation specialists improves functional outcomes. In cervical dystonia, consider adjunctive physical therapy and ergonomic changes.
For chronic migraine, maintain lifestyle supports: sleep regulation, hydration, and trigger management. Medication-overuse counseling is essential. Coordinate with neurology on preventives and acute therapies when indicated.
For hyperhidrosis, encourage breathable fabrics, antiperspirant routines, and stress-management techniques. Reassess impact on quality of life each cycle.
Product Families and Clinical Nuance
Different botulinum toxin formulations vary in excipients, units, and diffusion characteristics. Units are not interchangeable across brands. When switching between formulations, reset expectations and dosing plans based on evidence and experience.
For clinicians comparing categories, a brief overview of Botulinum Toxins can contextualize differences in onset, spread, and labeling. Always align product choice with indication, anatomy, and patient priorities.
Case Scenarios to Guide Planning
A 38-year-old with prominent glabellar lines seeks a natural look. Conservative dosing to corrugators and procerus, with careful brow elevator preservation, minimizes the risk of heaviness. Set a two-week review to assess symmetry and movement.
A 55-year-old post-stroke patient has wrist flexor spasticity impeding hygiene. Ultrasound-guided injections to specific flexors, followed by stretching and occupational therapy, target function over tone alone. Reassess range, pain, and caregiver burden at six weeks.
A 42-year-old with chronic migraine documents 18 headache days monthly. Structured injection mapping, diary tracking, and sleep hygiene can help quantify response. Coordinate with a neurologist for comprehensive preventive planning.
Safety Pearls and Risk Mitigation
- Screen for neuromuscular disorders and respiratory compromise before treating.
- Use the lowest effective dose in functionally sensitive muscles.
- Maintain appropriate dosing intervals to minimize cumulative weakness.
- Educate patients about realistic goals and potential transient effects.
- Document informed consent and emergency instructions for alarming symptoms.
Thoughtful planning and consistent follow-up improve outcomes while keeping safety central. Small, targeted adjustments often achieve better function and appearance than aggressive initial dosing.
Medical disclaimer: This content is for informational purposes only and is not a substitute for professional medical advice.For organization-wide standards and product navigation, visit MedWholesaleSupplies for additional clinical resources and category structures.
